Projects
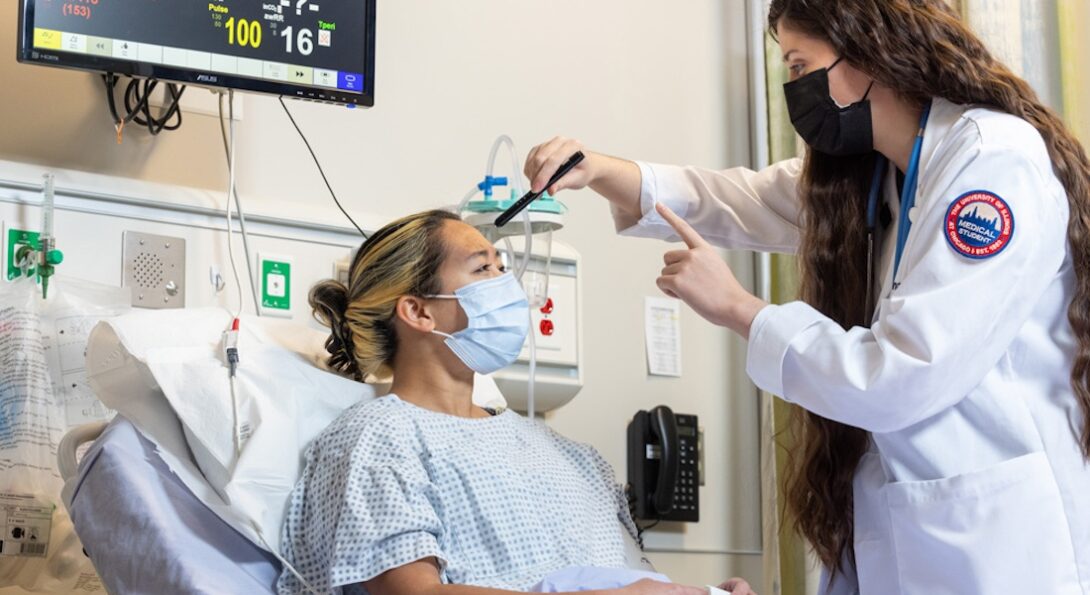
Clinical simulation provides compelling experiential learning programs and effective assessments of clinical skills.
Learn more about developing your own project at the center
Project Focus Areas Heading link
Column 1
- Technology-Based Simulation (Mannequin/Procedural Skills)
- Human-Based Simulation (Standardized Patient)
- Experiential learning
Real-life challenges are presented in a safe and supportive environment through the use of standardized patients, procedural task trainers (bench models), high-fidelity mannequins, virtual reality, and screen-based simulations. Experiential workshops combine lively interactivity with immediate debriefing, feedback, and coaching. - Assessment
Simulations allow valid and reliable assessments of key clinical competencies such as diagnostic interviewing, physical examination, communication, and interpersonal skills, decision-making, procedural skills, teamwork and professionalism. Digital video recordings document simulated encounters and can be reviewed, annotated and scored online.
Column 2
- Patient Safety and Quality Improvement
Simulations provide a safe venue for practicing new and error-prone procedures and investigating near misses. Unannounced standardized patients (“mystery shoppers”) provide a powerful tool for exploring the patient experience in hospitals and clinics. - Research and Innovation
Clinical simulation experiences serve as highly effective research interventions, outcome probes, and evaluation tools for research studies in health professions education and patient safety. The development and validation of new and innovative simulations is an additional area of scholarly activity. Programs are grouped under their primary learning or assessment objectives, although programs for advanced learners frequently address multiple objectives within a given simulated scenario. All programs can be modified for learners of different backgrounds and levels of training.
Program Objectives can Include: Heading link
- Communication Skills
- Interviewing and History-Taking Skills
- Physical Exam Skills
- Procedural Skills
- Team Training
- Patient Safety and Quality Improvement
- Research